 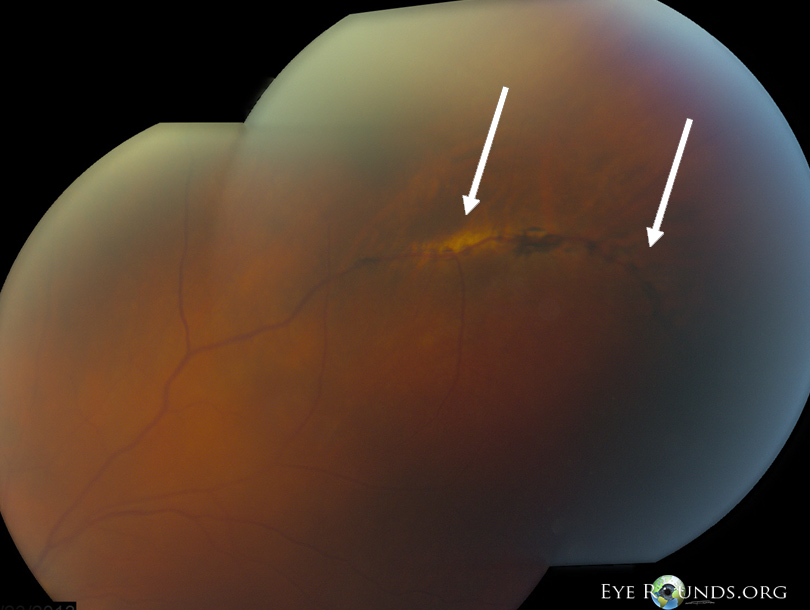
PLs not accompanied by LD may suggest a condition other than LD. 
Our preliminary observations suggest that this PL may coexist with typical LD in some cases. In our practice, we have noticed high incidence rates of pigmentary lesions in RRD eyes with flap tears, which may differ from those observed in typical LD, as pigmentary lesions (PLs) are often observed behind the retinal tears and may be located at the RPE or choroidal levels. These modalities have made it easier than it was before to evaluate and treat peripheral retinal lesions. In eyes with these pathological characteristics, the retina can be pulled as PVD progresses, leading to the development of retinal flap tear and RRD 16, 17, 20, 25, 26.Īlongside the wide-viewing systems in vitrectomy, ultra-widefield (UWF) imaging is commonly used in clinical practice 27, 28, 29, 30. Concentrated vitreous adheres to the margin of LD, and proliferated glial cells extend into the vitreous. Pathological findings revealed that the retina is thin in LD and loses its layered-structure, and that the inner limiting membrane is missing and replaced by retinal glial cells 16. Ophthalmoscopically, a typical case of LD presents with a white-striped appearance and slightly elevated margin 16, 17. Lattice degeneration (LD) is a retinal lesion associated with RRD 2, 6, 15, 16, 17, 18, 19 that is implicated in the onset of 20% to 65% of RRD cases 3, 4, 20, 21, 22, 23, 24. However, visual prognosis is poor in cases of RRD involving the macula, and those with re-detachment, long-term RRD, or RRD progressing to proliferative vitreoretinopathy. The visual outcomes of RRD have improved since adjuvant agents (e.g., triamcinolone acetonide 9, 10 and perfluorocarbon liquids 11, 12) and a wide-viewing system 13, 14 ecame available. In general, RRD with a flap tear rarely resolves on its own and requires surgeries in almost all cases 8. It is accompanied by a flap (horseshoe-like) tear and is associated with the progression of posterior vitreous detachment (PVD) 6, 7. Rhegmatogenous retinal detachment (RRD) is a representative vitreoretinal disease caused by a hole or flap tear in the retina 1, 2, 3, 4, 5. Pre-, intra-, and post-operative assessments of original flap tears suggested that PL might be a risk factor for RRD, developing alongside or separately from LD. In the retinal areas of 22 eyes, which were not affected by RRD, we observed PL without retinal tears some were accompanied by vitreous traction and tractional retinal detachment. On OCT, PL were located at the RPE level, while choroid abnormalities were unclear. In green FAF images, LD showed normal to mild-hyper fluorescence, whereas all PL showed hypofluorescence. Overall, 102 (88%), 63 (54%), 14 (12%), and 25 (22%) tears were accompanied by lattice degeneration (LD) or PL, both LD and PL, only LD, and only PL, respectively. A total of 116 retinal tears (mean count, 1.2 ± 0.5 range, 1–4 per eye) were observed in the detached retina. If PL did not involve RRD, we used OCT to preoperatively assess any pathologic changes to the lesion. We included 97 patients with unilateral rhegmatogenous retinal detachment (RRD) with posterior vitreous detachment who underwent vitrectomy, and examined pigmentary lesion (PL) characteristics around the sites of original tears using pre- and postoperative ultra-widefield scanning light ophthalmoscopy, green light fundus autofluorescence (FAF) imaging, and intraoperative digital video. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
